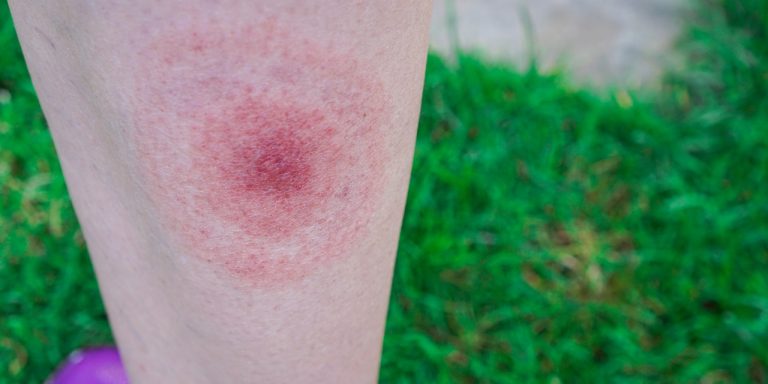
Tick bites: symptoms, treatment and long-term consequences
What does a dangerous tick bite look like? How long does a tick bite itch and remain visible for? Is redness after a tick bite normal? When should you consult a doctor? Find out more about tick bites, their treatment and possible consequences.
Overview of topics
What is a tick bite?
Ticks are a type of arachnid. They have eight legs and a round body. When ticks bite, they penetrate the top layer of skin with their mouthparts, usually on parts of the body where the skin is particularly soft. Tick bites are therefore often found on the ears, behind the knees and on the scalp. The armpits, the pubic area and the inner thighs are also often targeted. Ticks have small barbs on their hypostome (their “stinger”), which allow them to anchor themselves to humans and animals. While they do this, they release a secretion that, among other things, has an anti-inflammatory and anaesthetic effect. Ticks don’t bite immediately. Instead, they first crawl around the body and look for a suitable spot.
Ticks are usually active from March to November if the temperature is above 8 degrees Celsius. During this time, they live in damp, warm environments such as bushes, tall grass or undergrowth. In the winter months, however, they stay in the ground.
The term commonly used is “tick bite”, even though “tick sting” is actually more accurate. Ticks have a stinging and sucking apparatus. They use this to cut open the skin and attach themselves to it using barbs, before sucking out the blood via the hypostome.
Tick bites: symptoms
If the tick is not infected with pathogens, the tick bite causes few symptoms. If you remove the tick or it comes off on its own after about two days, you will probably notice a lump on your skin after it has bitten you. This tick bite is itchy, causes redness and is slightly swollen. It often takes several days or weeks for the lump and itching to disappear.
As a rule of thumb, if there is still no rash a month after a tick bite and you don’t exhibit any other symptoms, it is highly unlikely that the tick was infected with pathogens.
However, tick bites sometimes lead to an infection. In this case, it’s best to consult a doctor.
Sometimes a tick bite goes unnoticed because there are no obvious symptoms. Ticks release an anaesthetic secretion when they bite. That’s why the puncture site often doesn’t hurt. In addition, many people only notice a suspected tick bite once the tick has gone, so it’s often unclear whether the bite is a mosquito bite or a tick bite.
Disinfect the wound and monitor the area over the next few days. If you experience any complaints, consult a doctor.
Tick bites: what can you do?
Do you want to remove a tick correctly? Ideally, you should use a special card, fine, pointed tweezers or a special tick-removal tool. Grip the arachnid as close as possible to the bite site, ideally on its head. Slowly pull the tick straight out, in one smooth move. Check that you have removed the whole tick and that no mouthparts are left in the wound. Finally, you should disinfect the tick bite.
If you want to remove a tick, keep the following in mind:
- Do not twist or squeeze the tick, as this will leave the wound more vulnerable to infection.
- Do not burn the tick off or soak it in oil or alcohol.
- Remove the tick as soon as possible. If you don’t have a suitable tool to hand, remove the tick with your fingernails.
Treating a tick bite
In most cases, it’s not necessary to treat a tick bite. You can relieve any discomfort as follows:
- Cool the affected area of skin, for example using a compress or cool pack.
- Apply an anti-inflammatory ointment. A pharmacist can advise you on this.
- Support your body with measures that strengthen the immune system.
It’s a good idea to take a photograph of the tick bite while it’s still fresh. Repeat this every day. This allows you to see exactly how the skin area changes over time and keep an eye on any expanding rash (erythema migrans).
It’s worth noting that antibiotics are rarely needed in the event of a tick bite. Doctors only prescribe them if the bite causes complications.
In Switzerland, a tick bite is considered an accident. If you work more than eight hours a week for the same employer, their accident insurance also applies to you. So you should let them know. If you are not gainfully employed, for example because you are studying or drawing a pension, or if you work fewer than eight hours a week for the same employer and the accident is not work-related, your health insurer is responsible. Simply report your accident to us online via the myHelsana portal.
Tick bites: when should you consult a doctor?
Tick bites are usually harmless. But when are they dangerous and when should you speak to a medical professional? Seek advice if one of the following situations or symptoms occurs:
- You can’t remove the tick.
- You’ve already tried to remove the tick, but the tick’s head is still stuck in your skin.
- The tick bite leads to a red, ring-shaped rash rather than the normal redness.
- You suffer from flu-like complaints such as headaches after a tick bite. When do these symptoms occur? They can crop up a few days or weeks after a tick bite.
- You notice what is known as erythema migrans, an expanding rash. This appears 3 to 30 days after a tick bite and measures around 5 centimetres in size. It slowly becomes wider and is paler in the middle than at the edge. People with darker skin may also confuse erythema migrans after a tick bite with a bruise, as it can appear slightly bluish.
- Inflammation develops after the tick bite and the wound oozes pus.
- You suffer from diarrhoea, nausea, dizziness or vomiting after a tick bite.
- You have an allergic reaction after a tick bite, with symptoms such as a rash, constipation and nausea.
- You are immunocompromised or at particularly high risk. In this case, it is advisable to have your doctor perform a blood test. This allows them to determine whether you have been infected with Lyme disease and prescribe antibiotics as a preventive measure.
If you have a tick bite, monitor its appearance and progression. If you are unsure or experience any of the symptoms described above, be sure to consult your doctor.
Tick bites and children: when should you consult a doctor?
If your child only has the typical red and itchy lump after a tick bite, there’s no need to worry. However, watch out for symptoms such as headaches, fever, joint swelling or a reddened circle around the bite site. Just as for adults, tick bites rarely cause illness in children. However, talk to a paediatrician if the complaints persist for several days. The same applies if the symptoms appear only a few weeks or months after the tick bite.
If you have a tick bite during pregnancy, it’s best to consult a medical professional – especially if you notice any symptoms. A tick bite poses a potential risk to the unborn baby if you are infected with pathogens. Although it is rare for the unborn child to be infected, it is important to detect and treat an infection at an early stage.
Tick bites: long-term consequences
A tick bite can have various consequences. This is because some types of tick carry pathogens and, in rare cases, these can lead to illness.
Tick bites and Lyme disease
The bacteria that cause Lyme disease live in a tick’s midgut. The illness is caused by a tick bite when the pathogens from the tick’s midgut reach its salivary glands. After about 12 to 24 hours, the bacteria pass into the human body via the tick’s saliva. If doctors detect Lyme disease in good time, they can treat it effectively with antibiotics. There is no vaccination.
Tick bites and TBE
TBE (tick-borne encephalitis) is caused by viruses found in the tick’s saliva. These viruses can enter the human body shortly after being bitten. Although not every tick transmits the TBE virus and not every infected person becomes ill, in rare cases TBE caused by a tick bite can be fatal.
Tick vaccination
A tick vaccination protects against tick-borne encephalitis (TBE). The Swiss vaccination plan recommends this vaccination for all people who live in a high-risk area or spend time in one. In Switzerland, this applies to all cantons except Ticino. For people living in these areas, basic insurance covers the cost of the vaccination if it is administered by a doctor. Basic insurance does not cover vaccinations given in pharmacies.
Would you like to get vaccinated but basic insurance doesn’t cover the costs? In this case, supplementary insurance will come into play. With SANA, for example, you receive 75% of the costs of preventative measures such as vaccinations up to a maximum of CHF 500.– per calendar year. With COMPLETA, 90% of the costs are covered up to a maximum of CHF 750.– per calendar year.
It’s important to note that the vaccination only protects against TBE infection. You should therefore continue to follow tick protection measures to prevent you from contracting other illnesses that are transmitted by ticks.
Tick bites and alpha-gal syndrome
Some types of tick trigger alpha-gal syndrome by transferring the alpha-gal molecule with their saliva. Those affected have an allergic reaction to the sugar molecule galactose-alpha-1,3-galactose. This molecule is found in pork, beef, game, dairy products and gelatin, among other things. That’s why some people develop a meat allergy after a tick bite. They react to these foods with a rash, digestive problems, nausea and, in rare cases, anaphylactic shock.
Preventing tick bites in humans
Tick bite prevention involves various measures. These are particularly important if you spend time in areas with lots of ticks, for example if you go for a walk in the woods or a jog on narrow paths. Bear the following in mind:
- Wear closed-toe shoes, knee-length socks, long trousers and long-sleeved tops. Tuck your trousers into your socks.
- Choose light-coloured clothing and socks that will help you spot ticks faster.
- Spray your skin and clothes with insect repellent. Make sure that you observe the manufacturer’s instructions. These products are only partially effective and do not provide complete protection.
- Avoid walking through brush, bushes and tall grass. Run in the middle of paths.
- Do not sit on the ground or on stone walls.
- Thoroughly check your body and clothes for ticks after going for a jog or a walk. Bear in mind that ticks prefer warm and soft parts of the body such as the back of the knees, groin, armpits and scalp.
You should also talk to your doctor about the tick vaccination.
Tick bites are usually harmless. Be alert and protect yourself when you’re out and about. If you do notice a tick bite, keep a close eye on it for several weeks and discuss any complaints with a medical professional.

The expert provided the editorial team with advice and input for this article. Nadia Cifarelli (BSc Psychology, certified holistic health advisor) works for the Helsana health consultation service. She helps customers on issues to do with prevention, nutrition and mental health.

Newsletter
Find out more about current health issues every month and get all the information you need about our attractive offers from all Helsana Group companies * delivered by e-mail to read whenever it suits you. Our newsletter is free of charge and you can sign up here:
We did not receive your information. Please try again later.
* The Helsana Group comprises Helsana Insurance Company Ltd, Helsana Supplementary Insurances Ltd and Helsana Accidents Ltd.